|
T-scan (also called electrical impedance scanning or EIS) was approved by the U.S. Food and Drug Administration (FDA) in 1999 to be used as an adjunct tool to mammography in helping to detect breast cancer. T-scan uses the electrical impedance principal to measure the way electrical current passes through breast tissue and helps detect cancerous tumors. Conversely, T-scan imaging can also confirm when tumor tissue is benign (non- cancerous).
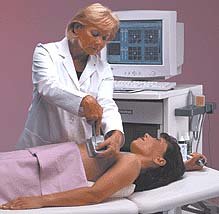
The T-scan measures low level bioelectric currents to produce real-time images of the electrical impedance properties of the breast. The resulting impedance images of the breast tissue can be used to help determine if the region of interest is normal tissue or a cancerous tumor. Supplementing mammography with T-scan imaging or other breast imaging exams (such as ultrasound) may reduce the number of unnecessary breast biopsies and create savings in healthcare costs. T-scan impedance imaging of the breast does not use radiation such as x-rays or radionuclides, does not require compression of the breast, and does not require an injection or biopsy sampling of the breast tissue via needle or surgical incision. T-scan impedance imaging is the first completely new imaging method to receive US Food and Drug Administration (FDA) clearance since magnetic resonance (also called MRI) imaging was approved in 1984. The T-scan works by creating an image "map" of the breast using a small electrical current. One-volt of continuous electricity (approximately the same as holding a flashlight battery by its ends) is transmitted into the body, either through an electrode patch attached to the arm or a hand-held cylinder. The electric current travels through the breast where it is then measured at skin level by a probe placed on the breast. The T-scan probe is similar to those used for ultrasound exams. Since cancerous tissue conducts electricity differently than healthy tissue, cancerous tumors may show up on the resulting images as bright white spots. A real-time image or "map" of the electrical properties of the breast is shown on the T-scan system monitor. X-ray mammography became clinically available in the early 1970s and is the gold standard in screening and breast cancer diagnosis. Mammography can detect approximately 85% of breast cancers and is the only FDA approved screening tool to help detect cancer in women with no signs or symptoms of the disease. However, mammography can miss up to 15% of breast cancers. A number of adjunctive tools including ultrasound, magnetic resonance and sestamibi nuclear medicine imaging have been developed to assist in determining when a breast biopsy may used in conjunction with mammography. T-scan breast imaging is a promising new development in breast cancer diagnosis. T-scan imaging, used in conjunction with mammography, may be more sensitive than mammography alone. As with every new medical test, multi-center clinical trials of the T-scan system were performed as part of the FDA approval process to evaluate the safety and effectiveness of this new modality. The results indicate that the T-scan is a cost-effective solution for increasing diagnostic accuracy and compliance for breast cancer diagnosis. As an adjunct to mammography, the T-scan may provide information for use in patient management and may help the physician determine whether or not to recommend biopsy. Other supplemental tests to mammography—magnetic resonance and nuclear medicine/sestamibi imaging of the breast—are both significantly more expensive and less patient friendly than T-scan imaging. Currently, T-scan is only available at approximately 35 facilities worldwide. As T-scan becomes more widely available, it may help to accurately diagnose more breast cancers in women. Updated: October 31, 2000 |